- Is toenail fungus prevalent in diabetics?
- What is the best way to clean diabetic toenails?
- Is toenail fungus caused by excessive blood sugar?
- What is the fastest technique to heal toenail fungus?
- Diabetics have thick toenails for a variety of reasons.
- Why are diabetics prone to fungal infections?
- What is the best way to cut thick diabetic toenails?
- With diabetes, how do you clip thick toenails?
- Is it necessary for diabetics to wear socks to bed?
- What is the best way to treat diabetic foot fungus?
- Why do diabetics have problems with their nails?
- Why are diabetics unable to clip their toenails?
- What is the white hard substance beneath my toes?
- What happens if you don’t cure toenail fungus?
- Is it necessary to remove my fungal toenail?
- What can I do to prevent my toenails from thickening?
- What can I do to restore the health of my toenails?
- Diabetics’ toenails turn black for a variety of reasons.
- Is metformin linked to fungus infections?
- What is the appearance of diabetic skin?
- What do diabetic legs look like?
- Is it okay for a diabetic to have a pedicure?
- Why cant diabetics put lotion between their toes?
- Why are diabetics unable to use wart removers?
- Is toenail fungus caused by type 2 diabetes?
- Should diabetics cut their toenails?
- Why should diabetics’ feet not be soaked?
- What are the characteristics of diabetic fingernails?
- Is it OK to use copper-fit compression socks if you have diabetes?
- What causes diabetics’ feet to swell?
- What can a diabetic’s feet soak in?
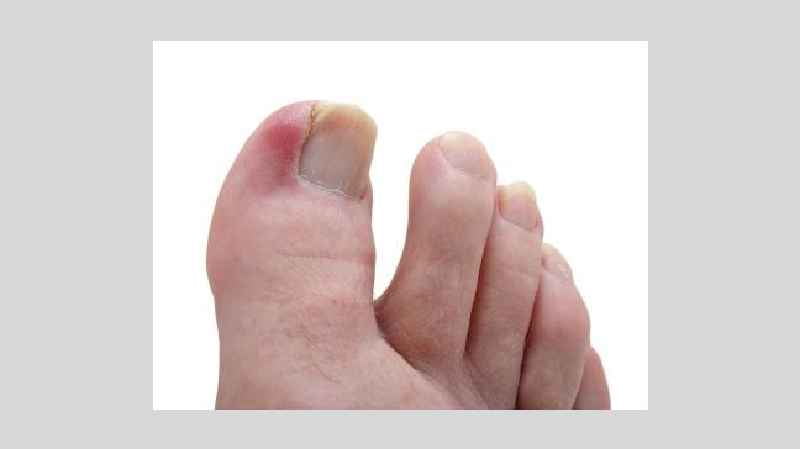
Is toenail fungus prevalent in diabetics?
For persons with diabetes, toenail fungus is a common foot condition. To prevent the fungus from spreading, consult a foot doctor for toenail fungus removal near Sugar Land as soon as possible if you get an infection.
What is the best way to clean diabetic toenails?
Instead of pruning your toes after a soak or shower, rinse them with warm water and a light soap, then dry completely before cutting. Keep an eye on the water temperature since diabetics with nerve loss may not be able to detect hot water and may burn themselves.
Is toenail fungus caused by excessive blood sugar?
Diabetes patients are more susceptible to toenail fungus infections and related consequences. It is very crucial to treat the infection and obtain appropriate glycemic control. (For people with diabetes, this isn’t only a cosmetic issue.)
What is the fastest technique to heal toenail fungus?
Medications.
- Antifungal medications taken orally. Because they eliminate the illness faster than topical treatments, these drugs are frequently the primary choice.
- Nail polish that has been medicated. Your doctor may prescribe ciclopirox, an antifungal nail polish (Penlac).
- Nail lotion that is medicated.
Diabetics have thick toenails for a variety of reasons.
Poor circulation is the most common cause of changes in diabetic toenails. Trauma – which, due to neuropathy, sometimes goes unreported. Susceptibility to fungal infections in general – caused by elevated blood glucose levels.
Why are diabetics prone to fungal infections?
Although this fungus is naturally abundant in our gastrointestinal systems and mouths, diabetes people are more likely to acquire an overgrowth, which can lead to a fungal infection. Because Candida albicans is so common, it is the major cause of fungal infections in both diabetics and non-diabetics.
What is the best way to cut thick diabetic toenails?
Toenails should be cut after a bath when they are soft. Trim them straight across, then file them smooth. Toes should not be sliced at the edges. Dont allow the corners of your toenails grow into the skin.
With diabetes, how do you clip thick toenails?
Always make tiny cuts rather than cutting the toenail all the way across. Cut straight across and smooth the edges with a nail file. Never apply lotion between the toes, only on the bottom and tops of the feet. Recommend that individuals with thickened or yellowed toenails get their toenails clipped by a foot care specialist such as a podiatrist.
Is it necessary for diabetics to wear socks to bed?
Consider socks designed exclusively for diabetic individuals. These socks have increased cushioning, do not have elastic tops, are higher than the ankle, and are constructed of moisture-wicking fibers. Toss on some socks before going to bed. If your feet are cold at night, wear socks.
What is the best way to treat diabetic foot fungus?
It has been demonstrated that terbinafine, itraconazole, and fluconazole have satisfactory cure rates. Recent studies have shown that topical therapy of the nail with 8% ciclopirox nail lacquer, bifonazole with urea, and amorolfine is effective.
Why do diabetics have problems with their nails?
Infections in and around the nails, such as Gram-negative bacteria or fungi, constitute a risk for people with diabetes. Neuropathy and glycaemia enhance the risk, as does injury to the nail or nearby skin, for example by deformed or sharp-edged nails. It’s critical to take care of your nails on both your hands and your feet.
Why are diabetics unable to clip their toenails?
Diabetes can cause nerve damage and numbness in your feet, which means you could be hiding a foot wound. Poor circulation makes healing more difficult, increasing your risk of infection and wounds that take longer to heal.
What is the white hard substance beneath my toes?
Nail psoriasis occasionally causes too much keratin to form under the nail. Subungual hyperkeratosis is the medical term for this outgrowth. Hyperkeratosis patients may see a white, powdery substance under their nails. When this happens to your toenails, the pressure of your shoes pressing down on your toes might cause pain.
What happens if you don’t cure toenail fungus?
If left untreated, fungal nail infections can make walking, exercising, and performing manual jobs like typing difficult. The main signs and symptoms of onychomycosis include: Broken and brittle.
Is it necessary to remove my fungal toenail?
If you have toenail fungus, your doctor will probably suggest one or more of the following treatments: Toenail Trimming is a procedure that involves removing the toenail and trimming it Sundling notes that while toenail trimming is normally done in conjunction with medication, getting the nail trimmed by a podiatrist on a regular basis is beneficial and allows the drug to operate better.
What can I do to prevent my toenails from thickening?
What are the options for dealing with thick toenails?
- Every day, wash the affected area with soap and water.
- Regularly groom your nails.
- After carefully filing your nails, use an over-the-counter fungal medication.
- Every day, apply Vicks VapoRub on your toenail.
What can I do to restore the health of my toenails?
10 Toe-Nail-Healthy-Growing-Tips
- Cleansing on a daily basis.
- Moisturize.
- Trimming on a regular basis.
- Filing.
- Diet that is good for toenails.
- Proper footwear and socks are required.
- Massage on a sporadic basis.
- Foot soaks are a great way to pamper yourself.
Diabetics’ toenails turn black for a variety of reasons.
Anemia, diabetes, heart disease, or kidney disease are examples of underlying medical conditions. Fungal infections: While they usually seem white or yellow, debris accumulation from fungal infections can sometimes result in black toenails.
Is metformin linked to fungus infections?
This medication has the potential to cause vaginal yeast infections in women and penis yeast infections in males. This is more likely in patients who have a history of vaginal yeast infections or in men who are not circumcised. A vaginal discharge, itching, or odor may occur in women.
What is the appearance of diabetic skin?
Small raised firm bumps that resemble pimples are common symptoms of this skin disorder. These pimples become bloated, hard patches of skin as time goes on. Yellow, reddish, or brown spots can appear.
What do diabetic legs look like?
The characteristic of diabetic dermopathy, often known as shin spots, are light brown, scaly patches of skin that commonly appear on the shins. Oval or circular patches are possible. Damage to the small blood arteries that deliver nutrients and oxygen to the tissues causes them.
Is it okay for a diabetic to have a pedicure?
However, if you have type 2 diabetes, you should be cautious about obtaining a pedicure because of the hazards associated. One is the risk of infection. Infection can elevate your blood sugar levels, interfere with appropriate healing and put you at risk of more serious consequences including ulcers and even amputation.
Why cant diabetics put lotion between their toes?
Apply a little layer of lotion, cream, or petroleum jelly on the tops and bottoms of your feet to maintain your skin smooth and silky. Avoid putting lotion or cream between your toes since moisture might lead to infection.
Why are diabetics unable to use wart removers?
Salicylic acid is used to cure warts, corns, and calluses without a prescription. It gently erodes the skin to eradicate the condition. However, if the patient has diabetes, salicylic acid could develop an infection from the skin erosion and the patient could lose a limb .
Is toenail fungus caused by type 2 diabetes?
If you have type 2 diabetes, you should be concerned about nail fungus. Diabetic feet are twice as likely to have toenail fungus, and severe instances, combined with comorbidities, can lead to amputations. If you have diabetes and find an issue with your nails, consult your doctor right once.
Should diabetics cut their toenails?
Myth: Diabetics are unable to clip their own toenails. This is not the case: The general guideline on toenail clipping applies to everyone. If you have diabetes, you should cut your nails to the form of your toes to keep them healthy. They should not be cut straight across, bent down the sides, or chopped too short.
Why should diabetics’ feet not be soaked?
If the skin on your foot begins to break down, you risk infection. Also, if you have nerve injury, be cautious about the temperature of the water. If you can’t tell if the water is too hot, you risk burning your skin.
What are the characteristics of diabetic fingernails?
The nails of some diabetics have a yellowish tint to them. This colour is frequently caused by the breakdown of sugar and its impact on the collagen in the nails.
Is it OK to use copper-fit compression socks if you have diabetes?
They are a non-invasive treatment option for diabetics who have poor circulation and nerve damage in their feet and legs. Compression socks help to improve nerve sensitivity while also preventing swelling from forming.
What causes diabetics’ feet to swell?
Poor blood circulation commonly causes swelling feet and ankles when you have diabetes. Excess fluid builds up in the bodily tissue, causing swelling in the feet and ankles. Edema is a type of swelling induced by an underlying condition like congestive heart failure, kidney illness, or diabetes.
What can a diabetic’s feet soak in?
It’s a mineral compound that’s sometimes used to treat tight muscles, bruises, and splinters at home. Epsom salt is sometimes used to bathtubs or tubs to soak in. Before bathing your feet in an Epsom salt bath, consult your doctor if you have diabetes.
Category:Skin & Nail Care