- Why is it vital for diabetics to take care of their nails?
- What does it mean to take care of diabetic nails?
- What nursing interventions should be given to the patient in order to prevent diabetic foot?
- What are the benefits of regular diabetic foot care?
- When you have diabetes, what happens to your nails?
- What is the significance of nail care?
- What are the risks of diabetic people having their nails trimmed?
- What can you do to avoid diabetes?
- Why are diabetics unable to trim their nails?
- What is the significance of foot care?
- How do you keep diabetic feet under control?
- What is the best way for men to take care of their feet?
- Which of the following is a diabetic foot care guideline?
- Is it possible for diabetes to cause nail infections?
- Is it safe for diabetics to wear nail polish?
- Are diabetics’ nails brittle?
- What is the best way to look after a nail patient?
- Why do clients need to be counseled on proper nail care?
- What services do you offer for nail care?
- What is the best way to offer a diabetic pedicure?
- Why are heating pads not recommended for diabetics?
- What is the best way to cut thick diabetic toenails?
- What is the best way to prevent type 2 diabetes?
- How may diabetes be prevented in its early stages?
- How do you teach a diabetic patient?
- What effect does diabetes have on your toes?
- What is Diabetic Foot, and how does it affect you?
- What is the best type of dressing for diabetic foot ulcers?
- What is the finest ointment for a diabetic wound?
- How could a diabetic foot ulcer be a complication?
- How can men maintain the health of their toenails?
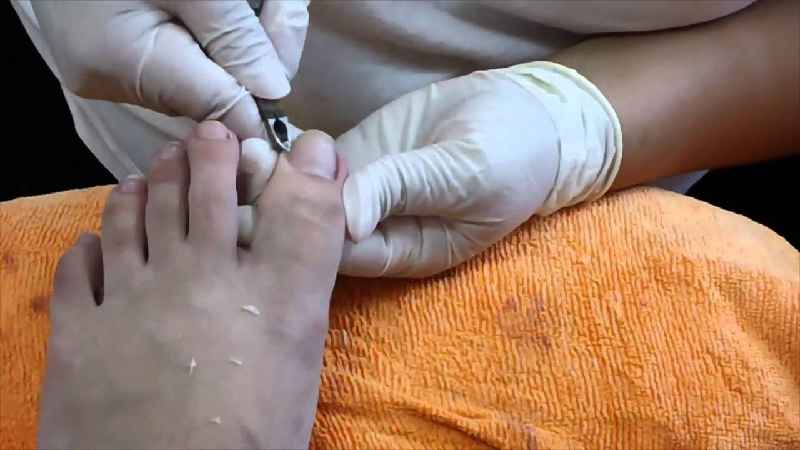
Why is it vital for diabetics to take care of their nails?
For everyone with diabetes, regular foot care (healthy skin, nail care, and proper footwear) is critical, as you have a higher risk of foot complications (such as skin that is dry and cracked, sores, changes in foot shape).
What does it mean to take care of diabetic nails?
At least once a year, visit your specialized podiatrist at Oklahoma Foot & Ankle Institute for diabetic nail care. Your podiatrist will do the following during these preventive exams: Examines your feet in detail. Trim your toenails in a straight line (if needed) Provides advice on how to thoroughly inspect your feet on a daily basis.
What nursing interventions should be given to the patient in order to prevent diabetic foot?
The feet of the patients should be washed, dried, and moisturized. When you’re done, make sure the water isn’t too hot and properly dry your feet. Lotion can be used on dry skin, but it should be avoided in the areas between the toes to avoid excessive wetness. Tell the patient that he or she should not walk barefoot.
What are the benefits of regular diabetic foot care?
Diabetes can be damaging to your feet, and even a little cut can have major implications. Diabetic foot care is vital. Diabetic nerve degeneration can result in the loss of feeling in your feet. Diabetes can also limit blood flow to the feet, making it more difficult to repair injuries and fight infections.
When you have diabetes, what happens to your nails?
Summary. Infections in and around the nails, such as Gram-negative bacteria or fungi, constitute a risk for people with diabetes. Damage to the nail or adjacent skin, such as deformed or sharp-edged nails, increases the risk, as does neuropathy and glycemia. It’s critical to take care of your nails on both your hands and your feet…
What is the significance of nail care?
Your nails serve as a robust shield for your hands while you labor with them every day, as well as a barrier – the cuticle – that keeps environmental toxins out. Regular, professional nail care ensures that your nails remain strong and capable of performing their functions.
What are the risks of diabetic people having their nails trimmed?
You can harm the sensitive tissue around your nails by cutting your nails too short, according to Williams. This can put someone with diabetes at risk of infection, especially if they have symptoms like neuropathy. When using scissors or clippers, or anything else that can cut or lacerate your skin, use caution.
What can you do to avoid diabetes?
Advertisement.
- Get rid of the additional pounds. Diabetes is less likely if you lose weight.
- Increase your physical activity. Regular physical activity has numerous advantages.
- Consume a variety of plant-based foods. Vitamins, minerals, and carbohydrates are all found in plants.
- Consume healthy fats.
- Make healthier choices instead of following fad diets.
Why are diabetics unable to trim their nails?
Diabetes can cause nerve damage and numbness in your feet, which means you could be hiding a foot wound. Poor circulation makes healing more difficult, increasing your risk of infection and wounds that take longer to heal.
What is the significance of foot care?
Work performance can be hampered by poor foot health, and time away from work can be lost as a result. You’re also less inclined to engage in physical exercise if your feet aren’t in good shape. As a result, there’s a larger chance of diseases including heart disease and diabetes, as well as decreased endurance and muscle mass.
How do you keep diabetic feet under control?
Diabetic Foot Care Suggestions
- Take good care of yourself and your diabetic condition.
- Every day, wash your feet in warm water with a gentle soap.
- Every day, look for sores, blisters, redness, calluses, or any other concerns on your feet.
- If your feet’s skin is dry, keep them moist by applying lotion after you’ve washed and dried them.
What is the best way for men to take care of their feet?
5 Tips for Men’s Healthy Feet
- Socks should be changed every day. Because feet sweat a lot during the day, it’s a good idea to change your socks once or twice a day to avoid excessive sweating.
- Soap and water should be used to clean your feet.
- Dry your feet completely.
- Toenails should be cut straight across.
- To solve an issue, don’t hack your foot.
Which of the following is a diabetic foot care guideline?
Blot or pat dry, paying special attention to the areas between the toes. Feet should be moisturized, but not between the toes. To prevent dry skin from itching or cracking, use a moisturizer on a daily basis. However, do not moisturize between the toes, as this might lead to a fungal infection.
Is it possible for diabetes to cause nail infections?
Diabetes patients are more likely than non-diabetics to get onychomycosis, a fungal infection. The toenails are commonly affected by this infection. The nails will become yellowed and brittle.
Is it safe for diabetics to wear nail polish?
A combination of chemicals found in everyday goods such as nail polish, fragrances, and toys has been linked to type 2 diabetes in adults over the age of seventy, according to a Swedish study. The presence of these compounds, known as phthalates, cannot be avoided.
Are diabetics’ nails brittle?
Diabetes’ lower-extremity complications are linked to impaired peripheral circulation, neuropathy, and immunopathy. Due to the absence of sensation in the feet, sharp brittle nails can puncture the nearby skin and go unnoticed, resulting in potentially life-threatening bacterial infections.
What is the best way to look after a nail patient?
How to care for a resident’s nails.
- Hands should be washed and gloves worn.
- To soften the inhabitants’ nails, soak their hands in warm water.
- Clean the filth from beneath your fingernails.
- Trim your nails straight across using a nail clipper. Using an emery board, round the edges.
- Apply lotion to your hands and fingers if desired.
Why do clients need to be counseled on proper nail care?
Dirt build-up can cause your nails to become brittle and undermine their integrity. It’s crucial to remember that even small amounts of debris and filth under your nails can spread illness, so washing your hands and nails more thoroughly isn’t only for you.
What services do you offer for nail care?
Services for nail care.
- Manicures.
- Pedicures.
- Overlays and extensions in acrylic.
- Overlays and extensions with UV gels.
- Dip your nails with powder.
- SNS has nailed it.
- Overlays and extensions in silk/fibreglass.
- Designing your nails.
What is the best way to offer a diabetic pedicure?
A Diabetic Client is being pedicured.
- Always inquire whether a client is diabetic.
- Don’t leave your feet in the water for more than five minutes.
- Allow the products to do the heavy lifting.
- Cuticle should not be sliced or pushed back.
- Use anti-microbial and urea-based hydrating products.
- Allowing the client to go without discussing maintenance is not a good idea.
Why are heating pads not recommended for diabetics?
The skin of older persons thins with age and is more vulnerable to harm when they have diabetes. When combined with diabetic neuropathy’s diminished sensitivity, a heating pad set too high can easily burn a senior’s sensitive skin. If your loved one insists on using heat to ease discomfort, you should try to persuade them otherwise.
What is the best way to cut thick diabetic toenails?
Toenails should be cut after a bath when they are soft. Trim them straight across, then file them smooth. Toes should not be sliced at the edges. Allowing the corners of your toenails to grow into the skin is not a good idea.
What is the best way to prevent type 2 diabetes?
What can I do to reduce my risk of having type 2 diabetes?
- It’s possible to lose weight and keep it off. By decreasing 5 to 7% of your starting weight, you may be able to prevent or delay diabetes.
- Increase your physical activity. 5 days a week, get at least 30 minutes of physical activity.
- Most of the time, eat nutritious things.
How may diabetes be prevented in its early stages?
Begin with these six suggestions:
- Sugar and processed carbs should be avoided in your diet. Consumption of foods high in refined carbs and sugar raises blood sugar and insulin levels, potentially leading to diabetes.
- If you’re a current smoker, you should quit.
- Keep an eye on your servings.
- Make a goal of 30.
- Drink plenty of water.
- Consume fiber.
How do you teach a diabetic patient?
Education and assistance.
- Make smarter diabetes-related decisions.
- Work with your medical team to get the help you require.
- Learn how to take care of yourself and how to: Eat a healthy diet. Take part in activities. Examine your blood sugar levels (glucose). Take your medicine as directed. Solve issues.
What effect does diabetes have on your toes?
Diabetes-related nerve damage can cause changes in the shape of your feet, such as Charcots foot. The symptoms of Charcots foot include redness, warmth, and swelling. Bones in your feet and toes can shift or crack over time, giving your feet an unusual shape like a rocker bottom.
What is Diabetic Foot, and how does it affect you?
Diabetes patients frequently experience foot difficulties. When high blood sugar destroys the nerves and blood vessels in the feet, they might develop over time. Diabetic neuropathy is nerve degeneration that can cause numbness, tingling, pain, or lack of feeling in your feet.
What is the best type of dressing for diabetic foot ulcers?
Nonadherent or saline-soaked gauze dressings are commonly used as a routine treatment for diabetic ulcers and are frequently used as the control arm in dressing studies. These dressings are intended to be atraumatic and to keep the wound moist.
What is the finest ointment for a diabetic wound?
When administered topically, antibiotics including Neomycin, Gentamycin, and Mupirocin provide strong antibacterial coverage. Silver-based dressings are available in a variety of compositions and provide excellent antibacterial protection. Diabetic foot wounds have responded well to silver dressings and polyherbal treatments [74].
How could a diabetic foot ulcer be a complication?
Diabetes mellitus causes severe atherosclerosis of the tiny blood arteries in the legs and feet, leading to vascular compromise and diabetic foot infections. Healing is slowed as a result of the lack of blood supply to the wound, eventually leading to necrosis and gangrene.
How can men maintain the health of their toenails?
Wash and dry your feet frequently, especially between the toes, where the culprits usually take hold. Replace your socks on a regular basis. Apply an antifungal lotion or powder to your skin. A wide range of brands are available in drugstores.
Category:Skin & Nail Care